Guide to assessing candidacy for in-office pediatric sedation
Dr. Emily Knipper offers guidance on assessing whether pediatric sedation is appropriate for young patients.
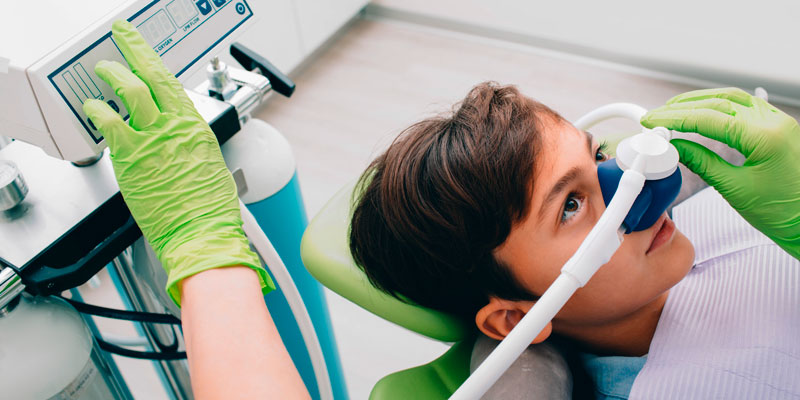
Dr. Emily Knipper offers a systems-based approach to in-office sedation
Although most dental work can be completed without sedation, children may require sedation for the completion of dental work if they have severe anxiety, special needs that challenge cooperative ability, young age, and/or extensive treatment. For children requiring sedation, dentists are faced with options regarding the type of sedation, who performs it, and the location of sedation. In-office IV sedation has the benefits of convenience for the dentist, staff, and patient, while the administration of IV medicine facilitates a predictable level of sedation. However, because of the potency of the medicines used and the in-office setting, selection of patients for this practice is key to ensuring safety. This article uses a systems-based approach to guide dentists in assessing a child’s candidacy for in-office sedation.
Neurological
A key consideration for assessing neurological pathology in this setting is to ask how a child’s neurological disease, if present, will affect his/her ability to recover from sedation in a timely and predictable manner. Neurological pathologies that are associated with weakness, such as myasthenic syndromes, are poorly suited for the office setting, because weakness can necessitate assistance with breathing during recovery, and an in-office setting may not be equipped to handle this for extended periods of time.
Seizures are not infrequently seen in children. A history of a single febrile seizure in childhood will likely have little effect on a child having sedation, but a history of poorly controlled and/or frequent grand mal tonic-clonic seizures raises concerns about safety in a dental office. Practical questions to ask are if the child has ever received a “rescue medicine” for a seizure and the type and frequency of seizures.
No matter the age, each child should receive a thorough evaluation and physical exam by an anesthesiology provider well-trained in pediatric pathology before being taken care of in an office setting, with ample time to assess any of the above conditions and to obtain records from specialists where applicable.
Cardiovascular
Cardiovascular health is key for the safety of in-office sedation. When considering a child with congenital heart disease, the type of defect, what repair has been done, and whether or not any further surgery is planned are key. Children with simple congenital heart disease, such as small ventricular septal defects with left-to-right shunting, may be considered for in-office sedation, on a case by case basis and depending on their functional status. Children with more complicated disease, and particularly that which has necessitated repair, are often more safely taken care of in an operating room setting. Specifically, any sort of congenital heart disease necessitating the “single-ventricle pathway” for repair should not be taken care of in the office (i.e., hypoplastic left heart syndrome, double outlet right ventricle, tricuspid atresia, mitral atresia). Even in their “repaired” states, the physiology in these children is tenuous, and perturbations to fluid and oxygen status can lead to rapid deterioration. In general, if a heart surgery has been done, it is important to ask what repair was done for purposes of determining the need for prophylactic antibiotics, as well as the child’s functional status, and if there are any issues with heart arrhythmias, breathing, and nutrition. A recent echocardiogram is key, as it allows assessment of shunting, valvular pathology, and ventricular function.
Respiratory
When assessing respiratory pathology, it is important to consider how it affects a child’s everyday life. For instance, asthma that is poorly controlled and frequently flares should likely be better controlled before considering in-office sedation. Bronchospasm or laryngospasm from reactive airways can quickly become life threatening. Obstructive sleep apnea is another pathology that affects a child’s everyday life and raises concerns about in-office care. Apnea or the need for supported ventilation during sedation can complicate care, prolonging recovery and increasing the chances of complications.
In-office sedation has the benefit of convenience and safety when careful consideration to patient selection is given. All body-systems are important in considering potential safety, but neurologic, cardiovascular, and respiratory concerns are frequently paramount. Of note, children with syndromes and any metabolic disorders (i.e., lysosomal storage disease, glycogen storage disease, mitochondrial disease), need to be carefully evaluated and are likely best taken care of in a hospital setting. Children who are at risk for aspiration due to delayed gastric emptying, severe acid reflux, or history of congenital defect (i.e., duodenal atresia as seen in Down Syndrome), should be identified and thoroughly evaluated.
Regarding age, no specific age cutoff has been delineated as unequivocally correlating with complications. However, individual anesthesia providers may vary in their facility with taking care of younger children, and providers with greater depth of pediatric training typically have more experience with younger children (i.e., under age 3 years old). Physiologic reserve is decreased in younger ages, making the margin for error in their care smaller. No matter the age, each child should receive a thorough evaluation and physical exam by an anesthesiology provider well-trained in pediatric pathology before being taken care of in an office setting, with ample time to assess any of the above conditions and to obtain records from specialists where applicable. Doing so preserves the safety of this unique and often convenient model of care.
 Emily Knipper, MD, attended medical school at Wake Forest University in Winston-Salem, North Carolina. She completed a residency in Anesthesiology at the University of Virginia in Charlottesville, Virginia, and completed a fellowship in Pediatric Anesthesiology at Seattle Children’s Hospital. She and her family live in Charlotte, NC, and she provides in-office sedation for children having dental work in North Carolina and South Carolina.
Emily Knipper, MD, attended medical school at Wake Forest University in Winston-Salem, North Carolina. She completed a residency in Anesthesiology at the University of Virginia in Charlottesville, Virginia, and completed a fellowship in Pediatric Anesthesiology at Seattle Children’s Hospital. She and her family live in Charlotte, NC, and she provides in-office sedation for children having dental work in North Carolina and South Carolina.
Disclosure: Dr. Knipper is a partner of Pediatric Dental Anesthesia Associates.
Adult patients must be assessed just as meticulously as pediatric sedation patients. Read “Dental Sedation: An Overview” in our sister publication, Implant Practice US at https://implantpracticeus.com/ce-articles/dental-sedation-an-overview/.
